Treatment Options for Peripheral Arterial Disease (PAD)
Lifestyle Changes, Medications and Surgery for PAD
When it comes to managing peripheral arterial disease, the main goal is improved blood flow through your arteries. Lifestyle changes and medications can be a big help. But when these aren’t enough to relieve your pain and symptoms, stenting and/or surgical procedures may be the key to finding relief.
Your doctor will recommend a treatment plan for you based on your symptoms, test results, medical history and future potential risks.
LIFESTYLE CHANGES AND MEDICATIONS
With lifestyle changes and/or medications, you may be able to avoid surgery or other procedures that involve additional health risks and high costs. These methods alone may not work to clear your arteries and control your peripheral arterial disease (PAD), but there are some important things your doctor may recommend.
- Lifestyle changes – PAD is common among smokers and people with diabetes. If you are a smoker, it is important to quit. If you have diabetes, take steps to lower your blood sugar. It’s also critical for those with diabetes and PAD to monitor and protect their feet from injury. With these conditions, there is a narrowing of the arteries that frequently leads to decreased blood flow to the legs and the feet, causing injuries to heal poorly. A healthy diet and exercise are other key lifestyle changes to help control PAD.
- Medications – Along with recommending lifestyle changes, your doctor may prescribe medications (pills) to slow the progress of the disease or to ease some symptoms. Some medications may be used to help control cholesterol, blood sugar, or blood pressure, while others may help prevent clots from forming within narrowed blood vessels. It’s important to note, that some medications can cause side effects you may not be able to manage, along with other health-related risks.
DRUG-COATED BALLOON ANGIOPLASTY
Drug-Coated Balloon (DCB) angioplasty is similar to plain old balloon angioplasty procedurally, but there is the addition of an anti-proliferative medication coating the balloon, as well as an excipient to aid in drug transfer, which may help prevent restenosis. Restenosis is the re-narrowing of the vessel at a site that was previously treated. Using a drug-coated balloon has the potential in prohibiting cell division, limiting the amount of restenosis, or blockage re-growth after treatment.
Learn more about Drug-Coated Balloon (DCB) angioplasty
BALLOON ANGIOPLASTY
Balloon angioplasty is done in the catheterization laboratory (“cath lab”). The doctor injects a special dye through a small, thin tube called a catheter into your bloodstream. The dye allows the doctor to view your arteries on an X-ray monitor. A device with a small balloon on its tip is then inserted through an artery in your leg or arm and threaded through the arteries until it reaches the narrowed area. The balloon is inflated to flatten the plaque against the wall of the artery, opening the artery and restoring blood flow. Then the balloon is deflated and removed from your body.
Learn more about Balloon Angioplasty
STENT THERAPY
Your doctor may recommend placing a stent to reopen your blocked artery. A stent is a small, expandable, mesh-like tube that supports the artery and helps to keep it open.
Learn more about Stent Therapy
OPEN SURGERY
There are several types of open surgery that may also be used to treat PAD. Two of the most common surgeries are endarterectomy and bypass.
Endarterectomy
An endarterectomy is a procedure that removes plaque directly from the inside of the artery wall. This is the preferred treatment when PAD is severe.
During this procedure, a doctor makes a small incision (cut) along the blocked or narrowed artery and physically removes the plaque. In some cases, the blocked portion of the blood vessel is also removed. After the plaque has been removed, the artery is closed with stitches or by a patch made from your own vein or synthetic material. Blood flow is then restored through the artery and the outer incision is closed. Patients usually stay in the hospital for one to two days to continue their recovery at home.
Benefits of endarterectomy:
- An endarterectomy is effective at restoring blood flow and relieving PAD symptoms.
- Treatment usually lasts many years.
Potential risks associated with endarterectomy:
- The artery may become blocked again (restenosis).
- You may experience temporary skin numbness and swelling around the incision site.
- The surgery requires conscious sedation or general anesthesia, which increases health risks.
- Complications like stroke, infection, and deep vein thrombosis are possible.
Bypass
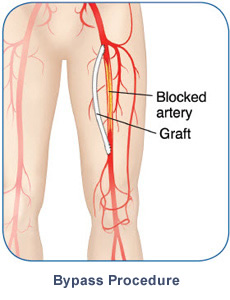 Your doctor may choose to do a bypass in more serious cases of PAD where blockages are very long or very hard (calcified). This procedure uses a graft – either a healthy blood vessel from another part of the body, or a synthetic tube – to reroute the blood flow around a blocked artery and create a new, permanent pathway for blood to flow.
Your doctor may choose to do a bypass in more serious cases of PAD where blockages are very long or very hard (calcified). This procedure uses a graft – either a healthy blood vessel from another part of the body, or a synthetic tube – to reroute the blood flow around a blocked artery and create a new, permanent pathway for blood to flow.
The procedure is done in a hospital under general anesthesia. The doctor makes a small opening near the blockage in the diseased artery. The graft is then attached (grafted) above and below the blockage, creating a new passageway for blood to flow (bypass) around the blocked artery. During the procedure, the doctor may do an angiography or ultrasound to check the bypass for any problems and to make sure it is working properly. Patients typically stay in the hospital for several nights and continue their recovery at home for two to three months.
Benefits of bypass:
- The surgery is effective at restoring blood flow and relieving PAD symptoms.
- Treatment usually lasts many years.
Risks associated with bypass:
- The surgery requires general anesthesia (you are not conscious during surgery), which increases health risks.
- The affected blood vessel could be injured.
- Your recovery time may be long.
- Infection is possible.
Information on this site should not be used as a substitute for talking with your doctor. Always talk with your doctor about diagnosis and treatment information.
